Posts Tagged ‘birth control’
Live Session at APhA 2026
Lights, Camera, Access: Contraception Care at the Pharmacy Recent policy changes have expanded pharmacists’ ability to provide contraception care, including prescribing hormonal, nonhormonal, and emergency contraceptives. We will discuss the…
Read MoreIs it Safe for Birth Control Users to Go Years Without a Period?
Is it Safe for Birth Control Users to Go Years Without a Period? Conversations about contraceptive options have grown more frequent—and often more polarized—on social media platforms. Contraception is commonly used…
Read MoreEnhancing Patient Understanding With Contraceptive Demonstration Kits
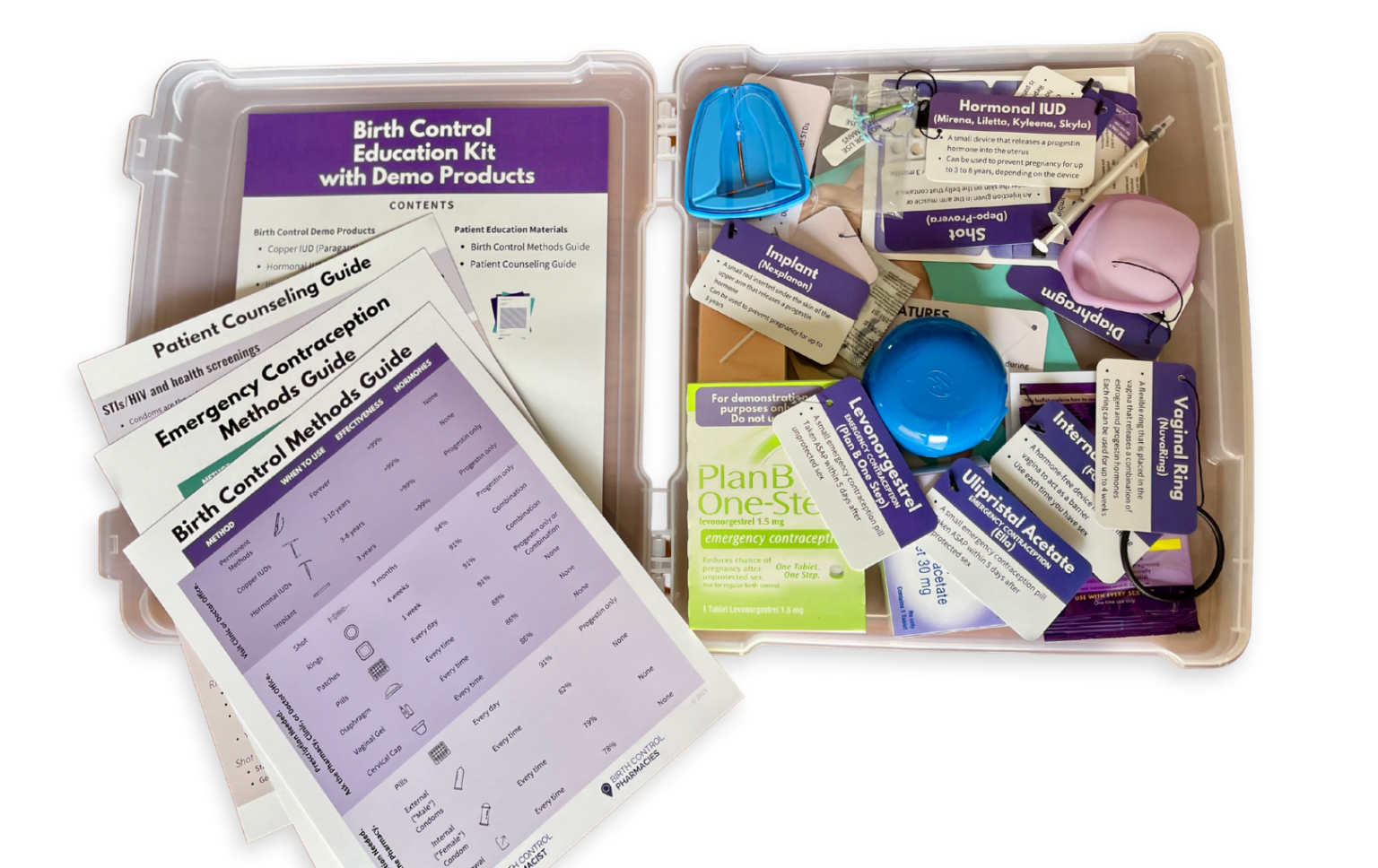
Dr. Ashley Meredith discusses how she uses the Birth Control Education Kit as a useful resource for patient counseling and engaging classroom instruction.
Read MoreComplex Contraception Cases – Live Webinar
Rescheduled – Join us on Wednesday, September 10th at 5-6 pm PT / 8-9 pm ET In this live webinar we will evaluate complex contraception patient cases, identifying key factors…
Read MoreContinuing Contraception Care After Trump’s Orders
In light of recent actions over the last two weeks with our new administration, I wanted to provide updates and guidance to my pharmacist peers regarding reproductive health care. On…
Read MoreFounder Reflections on 2023
As I reflect on this past year, 2023 finally brought us some wins in reproductive health. And I personally had the opportunity to contribute to landmark steps forward. ⭐️ The…
Read MoreOver-the-Counter Birth Control Pills: FDA Considering HRA Pharma’s Opill
Why Over-the-Counter Birth Control? Oral contraceptives have been around since 1960, and their risks and safety profiles have been well-studied throughout the years. According to the Guttmacher Institute, unplanned pregnancies…
Read MoreUpdated Report on State Policy Efforts to Expand Access to Contraception in Pharmacies
Download free 22-page report describing the current landscape of direct access to contraception in pharmacies, state policy approaches and experiences, as well as implementation.
Read MoreLevonorgestrel Intrauterine Device for Emergency Contraception
A new research study evaluates levonorgestrel IUD for emergency contraception
Read MoreMeet Phexxi – A New Non-Hormonal Contraceptive Gel
About the Product Lactic acid, citric acid, and potassium bitartrate (Phexxi, Evofem Biosciences) is a prescription combination, non-hormonal contraceptive gel approved by the FDA in May 2020. The vaginal gel…
Read More